
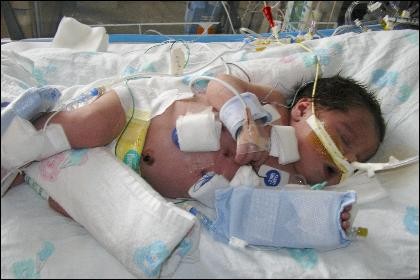
“If it can be done, it can be done here.” I find great comfort in the saying displayed over the Cardiac Reception Center’s Wall at the Children’s Hospital of Philadelphia or CHOP for short.
Samaria’s journey with a Complex Congenital Heart Defect can be summarized in twenty words-Three Open Heart Surgeries, Reconstruction, Three Heart Catheterizations, coding, CPR, doctors, nurses, specialists, feeding issues, medications, allergies, oxygen issues and HOPE.
At 24 weeks into pregnancy I had an ultra sound at our local hospital to determine the sex of our baby. I was not prepared to be told our baby’s one side of her heart was significantly enlarged and it would either stay the same or get worse. Samaria was prenatally diagnosed with a Complex Congenital Heart Defect, specifically Severe Ebstein’s Anomaly of the tricuspid valve with Pulmonary Atresia. The right side of her heart was enlarged due to the tricuspid valve not functioning properly.
We received sound advice with regards to Children’s Hospital of Philadelphia. A local maternal fetal medicine doctor told us, “Take ANY appointment they can give you.” This was the best advice we received and it is why we are so lucky we have our little girl alive and well today.
We went to the Cardiac Center at the Children’s Hospital of Philadelphia. The Fetal Heart Team led by Dr. Jack Rychik told us the baby was safe while I was pregnant because I was doing all of the work. The challenge would come once Samaria was born. The doctors at CHOP said they would wait and see after her birth if she would be strong enough to survive surgery to reconstruct her heart. If she fell into the 50% mortality category, she would go on the heart transplant list.
Born April 4, 2007, Samaria entered the world at the Hospital of the University of Pennsylvania, stabilized, and then sent to the Cardiac Intensive Care Unit at CHOP due to her life-threathening condition. The doctors gave Samaria a medication to prevent her patent ductus arteriousus (PDA) from closing. After observation, the plan was set into motion.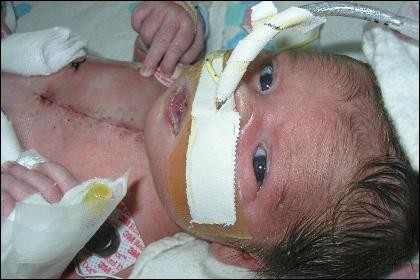
At just 5 days old, Samaria underwent the first of three surgeries at CHOP. Her surgeon, Dr. Thomas Spray, made the right side of her heart inactive and placed a shunt to redirect the blood flow. The road to recovery was long. We were delighted when Samaria was moved from the CICU to their step down unit. Unfortunately, Samaria had coded. The doctors responded quickly and performed CPR for 15 minutes. Our little girl was a fighter and pulled through.
After five weeks from being in the hospital from birth, we were able to bring her home! We arrived home with 5 different medications and a special diet of fortified breastmilk. Samaria had an NG tube for food and medicine. An NG Tube is a tiny little tube that is taped to her cheek which enters her body through her nose and goes down into her stomach. Samaria needed more calories, so pumped breast milk was mixed with concentrated formula to overcome the challenge that children with heart conditions have with gaining weight.
In June, while at her Pediatric Cardiologist Dr. R. Lee Vogel follow-up appointment, we were immediately sent back to CHOP as Samaria’s Oxygen level dropped to 60%. They performed a heart catheterization and were able to open up her shunt where it had narrowed. We left the hospital with Samaria on oxygen to keep her blood oxygen levels at 80%.
She had her NG Feeding tube removed in July 2007. 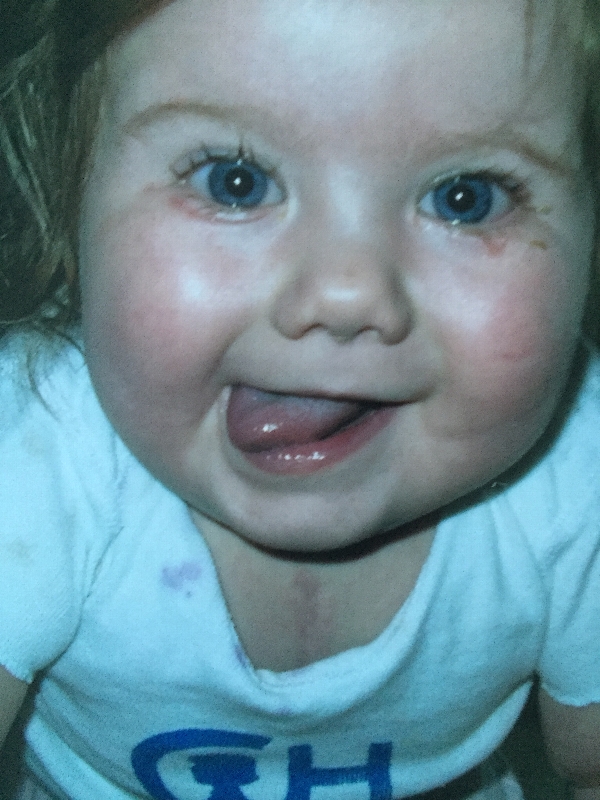 Five months old in August, Samaria had her second stage surgery, the Bi-directional Glenn Procedure. The second stage surgery went smoothly and we were surprised to be sent home in less than a week.
Five months old in August, Samaria had her second stage surgery, the Bi-directional Glenn Procedure. The second stage surgery went smoothly and we were surprised to be sent home in less than a week.
The Fontan was her third stage open heart surgery in October 2008, which left her with only two left side chambers. The oxygen poor blood goes directly into her lungs, collecting oxygen, entering the left side of her heart before pumping to her body.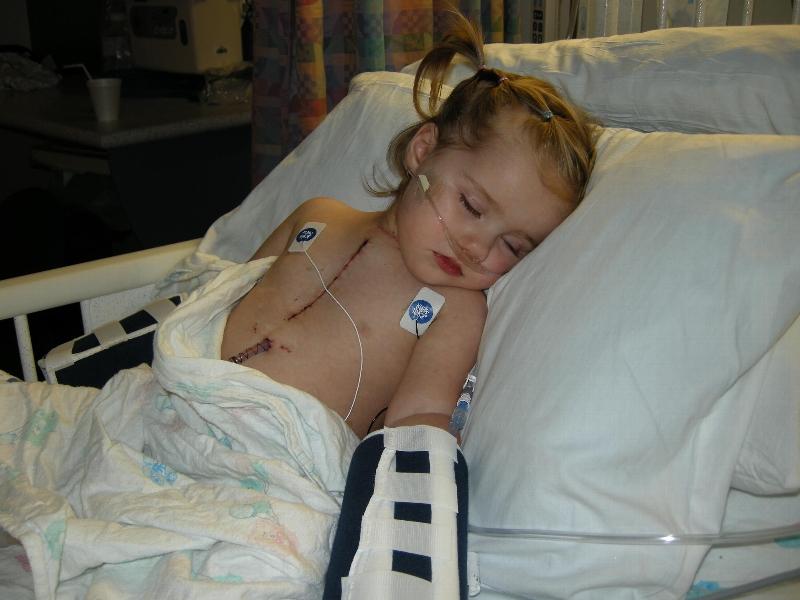




Samaria is now an eleventh grader who enjoys Girl Scouts, school clubs and jigsaw puzzles. In February 2015 we began the Single Ventricle Survivorship Group led by Dr. Jack Rychik. Through CHOP's continued evolution, it has changed into the Fontan Rehabiliation, Wellness, Activity and Resilience Development (FORWARD) Program. Forty years ago children with complex congenital heart defects didn't survive. Due to advances in medicine, these children are living with reconstructed hearts into their twenties and thirties. The professionals at CHOP are now finding our child's life saving palliative surgeries are the origin of many future problems. Exercise intolerance, arrhythmias, clotting, liver scarring, bone health, growth development, protein losing enteropathy, and plastic bronchitis are some of the many issues facing a single ventricle person. Research is critical to the quality and duration of these precious survivors.
There are challenges ahead of us, but the Children’s Hospital of Philadelphia is a magical place and HOPE LIVES HERE!
Join us in raising money for Single Ventricle Research at the Children's Hospital of Philadelphia. Every donation makes a difference! Thank you! Samaria is a dream come true! God Bless the Children's Hospital of Philadelphia!


Get The Word Out
https://chop.donordrive.com/campaign/samariamartin